“Barcodes” help gold nanoparticles to strike cancer energy centres
A new high-throughput platform screens dozens of nanoparticle designs in living systems to identify those that reach tumour mitochondria, enabling more precise and effective cancer therapies.
Researchers at the National University of Singapore (NUS) have developed a high-throughput method to identify gold nanoparticles capable of delivering therapies to the energy centres of cancer cells. By tagging nanoparticles with unique DNA ‘barcodes‘, the team was able to track and compare dozens of designs simultaneously in living tumour models, rapidly identifying those most effective at reaching this critical subcellular target.
The approach enables researchers to systematically evaluate how nanoparticle design, including shape, size and surface chemistry, influences their ability to accumulate in tumours and reach mitochondria.
Among the candidates tested, two formulations emerged as standout performers. One, a folic acid-modified cubic gold nanoparticle, achieved 99 per cent tumour regression in preclinical studies when used in a combined treatment involving mitochondria-targeted RNA therapy and mild photothermal therapy.
Led by Assistant Professor Andy Tay from the Department of Biomedical Engineering at the College of Design and Engineering and the Institute for Health Innovation & Technology at NUS, the study demonstrates how large libraries of nanomaterials can be screened efficiently inside living systems, providing a rational framework for designing nanoparticles that deliver drugs with far greater precision.
The study was published in Advanced Materials on 17 February 2026.
A barcode system for navigating the body
Mitochondria are attractive targets in cancer therapy because they regulate key processes such as energy production and programmed cell death. Delivering drugs directly to these organelles can disrupt tumour metabolism and trigger cancer cell death.
However, nanoparticles must overcome a series of biological barriers before reaching mitochondria: travelling through the bloodstream, entering tumours, penetrating cells and escaping cellular compartments that would otherwise degrade therapeutic cargo.
“Getting nanoparticles to the right place inside the body involves putting them through a complicated obstacle course,” said Asst Prof Tay. “Harnessing DNA barcodes enables us to track many nanoparticle designs simultaneously in living systems and quickly identify which ones can jump through various biological hoops successfully.
“In the study, each gold nanoparticle formulation was tagged with a unique DNA sequence, allowing the researchers to trace its distribution using next-generation sequencing. The team tested a library of 30 nanoparticle designs that varied in shape, size and targeting ligands.
After administering the pooled nanoparticles to tumour-bearing preclinical models, the researchers analysed where each design accumulated from whole organs to specific tumour cell types and ultimately to mitochondria.
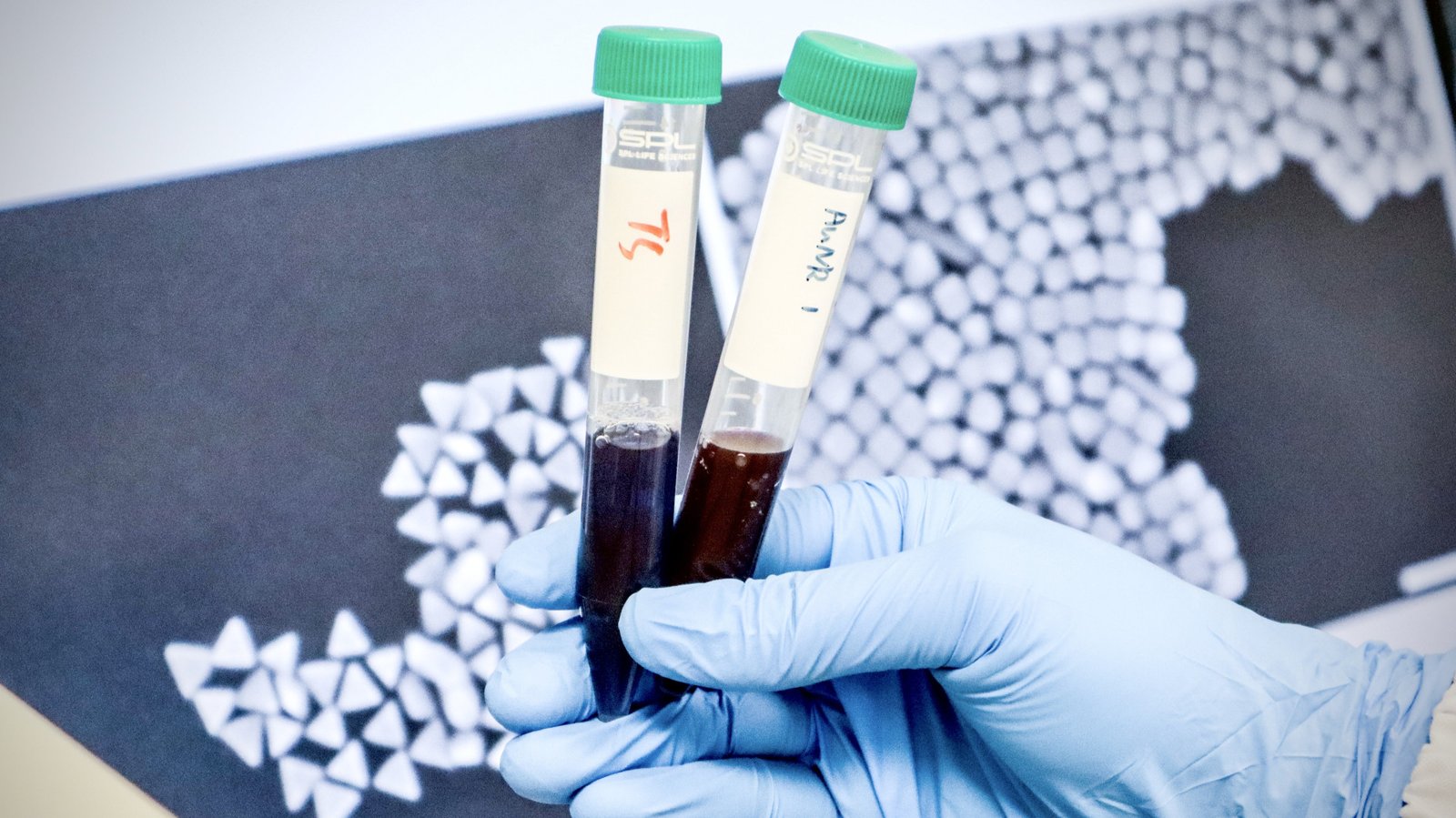
This multiplexed approach generated more than 1,000 in vivo data points while requiring around 30-fold fewer in vivo models than conventional one-by-one screening experiments. The work builds on the team’s earlier study published in November 2024, which first demonstrated the use of DNA barcoding to track nanoparticle bio-distribution in tumours.
While the previous study compared six nanoparticle designs at the tissue level, this new one greatly expands the library and extends the platform to analyse behaviour at cellular and sub cellular scales.
“The results revealed an important insight: nanoparticles that accumulated efficiently in tumours were also far more likely to reach mitochondria,” added Asst Prof Tay. “In other words, successful tumour targeting appears to be a prerequisite for effective sub cellular delivery.
“Among the nanoparticle formulations tested, two caught the team’s attention. Large spherical particles modified with folic acid accumulated strongly in tumours, partly due to a protective protein layer that prolonged circulation in the bloodstream.
Meanwhile, large cubic nanoparticles entered tumour cells more efficiently through clathrin-mediated endocytosis a cellular uptake pathway enabling effective mitochondrial delivery.
A step towards precision nanomedicine
To explore the therapeutic potential of these findings, the researchers tested the cubic nanoparticle formulation in a combined treatment strategy.
The particles were engineered to deliver small interfering RNA (siRNA) that disrupts mitochondrial gene expression, while also generating heat under near-infrared light through photothermal therapy. This dual approach produced strong anticancer effects in preclinical studies.
When applied together, the treatments led to almost complete tumour elimination after a single dose. Beyond killing cancer cells directly, the nanoparticles also interacted with tumour-associated macrophages (immune cells that normally support tumour growth).
The therapy appeared to shift these cells toward a tumour-fighting state, suggesting the approach may help reshape the tumour immune environment. “Our findings show that nanoparticle design is not governed by a single factor such as shape or size,” added Asst Prof Tay.
“Instead, multiple properties interact in complex ways. High-throughput screening platforms like ours allow us to uncover these relationships and move beyond trial-and-error in nanomedicine design.
“The platform could accelerate the development of precision nanomedicine by enabling researchers to rapidly identify nanoparticle designs suited for specific biological targets.
Potential applications include targeted delivery of RNA therapies, gene-silencing treatments and photothermal agents for cancer and other diseases.
Looking ahead, the research team plans to expand the nanoparticle library further and integrate automation and artificial intelligence tools to analyse the large datasets generated by the screening platform.
The researchers also aim to extend the method to target other cellular organelles, opening new possibilities for highly specific drug delivery within cells.researchers discovered a surprising phenomenon in optical physics that could lead to a faster and more precise biomedical imaging technique.
They found that under certain conditions, a chaotic mix of laser light can spontaneously organize into a highly focused “pencil beam.
“Using this self-organized pencil beam, the team captured 3D images of the human blood-brain barrier 25 times faster than the standard method, while keeping the same level of detail.
This technology allows scientists to see individual cells absorbing drugs in real-time, which could help test new treatments for diseases like Alzheimers and ALS to see if they reach the right parts of the brain faster and more clearly.
Sixian You, an assistant professor at MIT, explained, “The common belief in the field was that increasing the laser power would make the light more chaotic. But we proved that’s not true.
We followed the evidence, embraced the uncertainty, and found a way to let the light organize itself into a novel solution for bioimaging.”The discovery began with an observation that initially confused the researchers.
The team had developed a fiber shaper that allowed them to carefully adjust laser light passing through a multimode optical fiber. Cao was testing the fiber’s limits by increasing the power.
Typically, more power makes the light more scattered, but Cao noticed that as he approached the fiber’s limit, the light instead collapsed into a single, sharp beam.
To replicate this effect, the researchers had to follow two specific conditions. First, the laser had to enter the fiber at a perfect angle, zero degrees. Second, the power had to be increased until the light started interacting with the fiber’s glass.
“Once the laser reaches this critical power, the nonlinearity balances the fiber’s natural disorder, creating a stable, ultrafast pencil beam,” Cao explained.
Most researchers avoid high power levels to prevent damaging the fiber, and precise alignment isn’t often necessary because multimode fibers can carry so much power.
However, together, these techniques can produce a stable pencil beam without complex setup.
“This method is neat because you can use a normal optical setup without needing deep expertise,” You said.The pencil beam proved more stable and high-resolution than other beams, which often have “sidelobes” blurry halos that can mess up images. Their beam was clean and sharply focused.
Using this pencil beam, the researchers demonstrated its use in imaging the human blood-brain barrier, a tightly packed layer of cells that protects the brain but also blocks many medicines. Scientists and doctors want to see how drugs move through this barrier and reach their targets in the brain.
With standard methods, researchers can only capture one 2D section at a time and repeat the process multiple times. The new technique allows real-time tracking of how cells absorb proteins, creating ultrafast, high-precision images.
Roger Kamm, a professor at MIT, said, “The pharmaceutical industry is really interested in using human-based models to find drugs that can cross the barrier, as animal models often don’t predict what happens in humans. That this new method doesn’t require fluorescent tags is a game-changer.
For the first time, we can now visualize the time-dependent entry of drugs into the brain and even measure how fast different cell types take in the drug.”
“Importantly, however, this method isn’t just for the blood-brain barrier. It allows for tracking different compounds and molecules across various tissue models over time, making it a strong tool for biological engineering,” Spitz says.
The team created 3D images of cells that were better quality than with other methods, and they produced these images about 25 times faster.
“Normally, there’s a tradeoff between image clarity and how deep you can look at once — you can’t go too deep at the same time.
But with our method, we can beat this tradeoff by creating a pencil-beam that has both high clarity and a wide depth of focus,” You explains.
Looking ahead, the researchers want to better understand the basic physics behind the pencil-beam and how it self-organizes.
They also plan to use the technique in other situations, like imaging brain neurons, and work toward making the technology available for commercial use.
“You’s group created a beam that focuses energy in both time and space, which could be useful for microscopy that relies on light intensity.

They showed this and found it better than regular laser beams for imaging. It would be interesting to fully understand how these new pencil beams are made, as they could be useful in many imaging applications,” says Frank Wise, the Samuel B. Eckert Professor of Engineering Emeritus at Cornell University, who wasn’t involved in this work.
Source: National University of Singapore (NUS)